Cancer has long been viewed as a disease that largely affects people later in life. However, new findings from the Evernorth Research Institute shows that assumption is increasingly outdated – with real consequences for patients, employers, and the health care system.
The 2026 Health Care in Focus report finds that younger working‑age adults are accounting for a growing share of new cancer diagnoses, often with different cancer types, higher long‑term costs, and broader life disruption than previous generations experienced at the same age.
“Cancer is affecting more people during their working years,” said Kasey Raetz, PharmD, vice president of product and pharmacy contracting and strategy at Evernorth. “This has implications not just for health outcomes, but for workforce participation, financial stability, and long‑term employer planning.”
That shift is changing not only who is diagnosed, but how cancer care needs to be delivered across the entire journey – from early detection to long‑term support.
“These are not just earlier diagnoses of the same cancers we’ve always seen,” said Roseleen Charania, MD, associate chief medical officer for oncology programs at Evernorth. “We’re seeing different patterns, different needs, and much longer care journeys – which means our approach to prevention, care, and support has to evolve.”
Younger adults are driving growth in new diagnoses
Analyzing claims data from 2020 to 2024, Evernorth researchers found that while most cancer diagnoses still occur after age 50, the fastest growth of new cases is among younger generations.
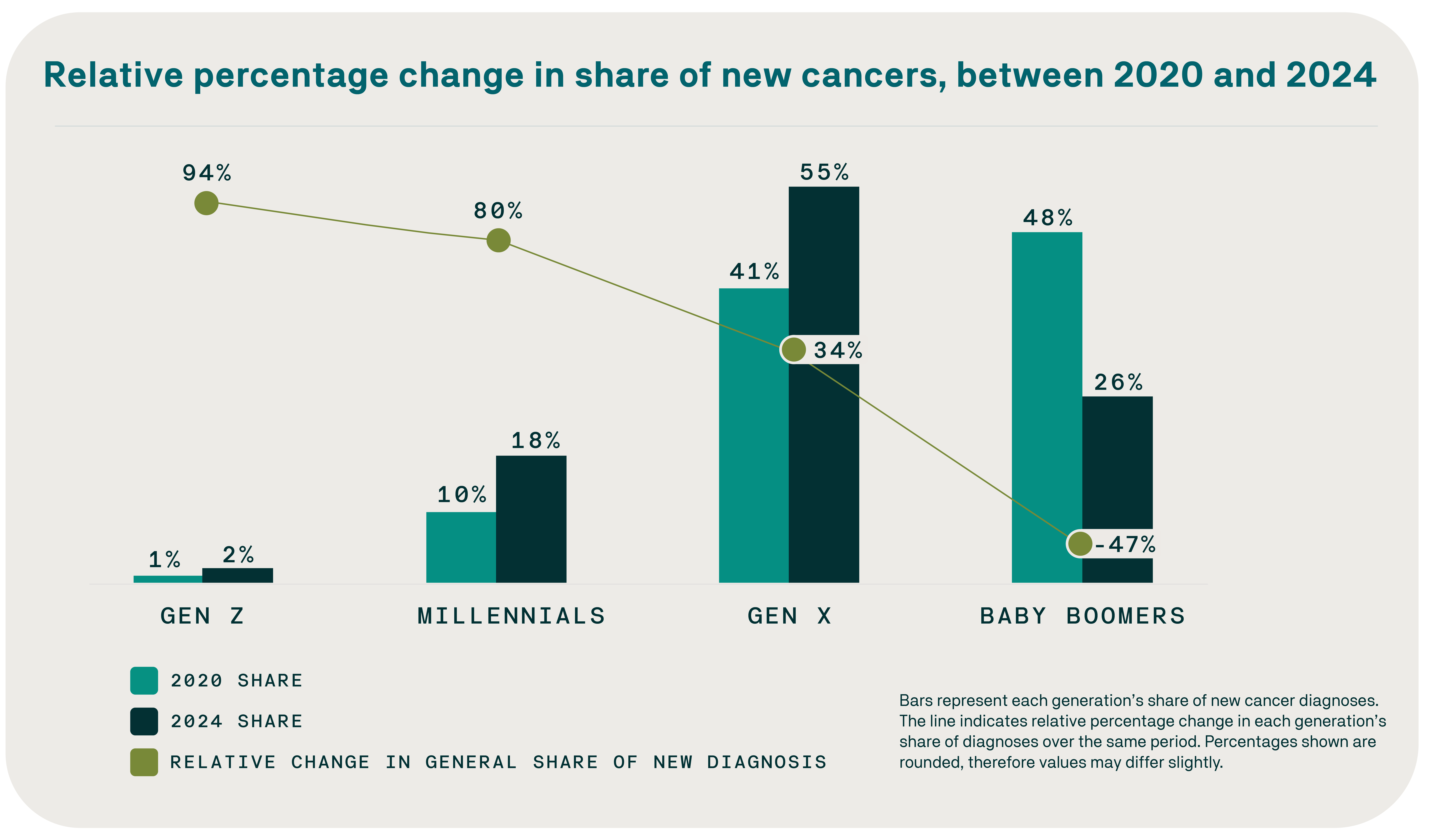
Gen Z and millennials have the highest increases in new cancer diagnoses (94% and 80%, respectively) than Gen X (34%), while the rate decreased for baby boomers (by 47%).
The relative share of new cancer diagnoses nearly doubled for Gen Z adults and rose sharply among millennials, even as it declined among Baby Boomers who are aging out of employer-sponsored coverage. Younger adults also present with a distinct mix of cancers, including higher rates of thyroid, colorectal, lymphoma, brain, and other less common malignancies – many of which lack routine screening pathways.
“For clinicians, this challenges the idea that age alone should determine risk,” Charania said. “When younger patients present with vague or unexpected symptoms, cancer is not always top of mind – and that can delay diagnosis and treatment.”
The impact of cancer extends far beyond treatment
For younger adults, cancer often collides with major life milestones – building a career, raising children, paying off debt, or achieving financial independence. The report’s survey data show that this intersection amplifies the burden of disease well beyond clinical care.
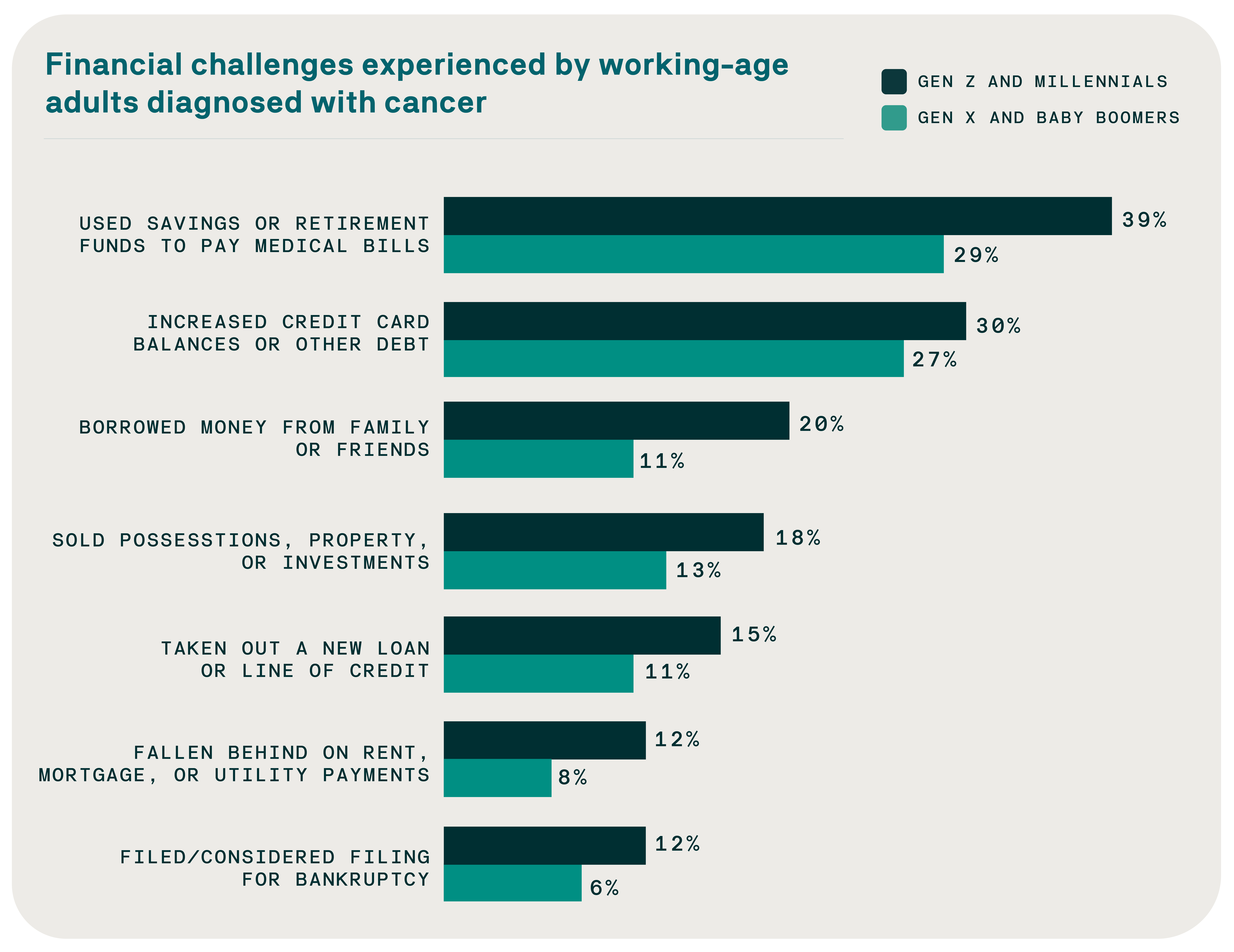
Nearly three‑quarters of Gen Z and millennial respondents reported financial stress related to cancer, and more than one‑third spent at least 10% of household income on out‑of‑pocket costs. Many tapped savings, borrowed money, or delayed basic expenses. About 1 in 5 said cancer significantly disrupted their ability to work.
“When cancer occurs earlier in working life, its impact extends into productivity, retention and long‑term workforce stability,” Raetz said. “Employers will need to reexamine their health benefit plans and workplace support strategies.”
Charania added that younger cancer patients are balancing treatment with work, caregiving, and financial pressure all at once. “If we focus only on chemotherapy schedules or clinical outcomes, we miss what actually determines whether someone can complete treatment and achieve recovery,” she said.
Caregivers – often spouses, significant others, parents, or friends – play a critical role yet frequently lack formal support. While family and community are central to the cancer journey, the report found that caregivers experience lost income, stress, and declines in their own health, with uneven support from employers.
A real‑life example of the challenges younger patients face
The findings mirror the personal experience of Adam Kautzner, PharmD, president of Evernorth Care Management and Express Scripts, who was diagnosed with melanoma in his early 30s.
After his cancer progressed to stage IV, Kautzner was told his best option was a clinical trial – one he ultimately found hundreds of miles from home. The treatment saved his life, but navigating the system while facing a life‑threatening illness left a lasting impression.
“Even with industry knowledge and resources, it felt like being dropped into a maze without a map,” Kautzner said. “I was trying to stay alive while figuring out where to go, how to get care, and how to make it all work.”
Now cancer‑free, Kautzner’s experience underscores a central theme of the report: access, navigation, and support can be just as critical as medical innovation itself – especially for younger adults and those living outside major care centers.
“There are people across the country who don’t have the ability to travel for treatment or advocate for themselves the way I could,” he said. “That gap in access is something we can and should address.”
Earlier diagnosis means longer care and higher lifetime costs
While younger adults represent a smaller share of total cancer cases, the report finds they generate higher average annual costs than older generations – and those costs accumulate over decades.
From 2020 to 2024, average annual per‑person cancer costs rose fastest among Gen Z and millennials, driven in part by cancers that require complex, multimodal treatment and long‑term follow‑up. Earlier onset also means longer engagement with the health care system, from survivorship care to mental health support, fertility preservation, and rehabilitation.
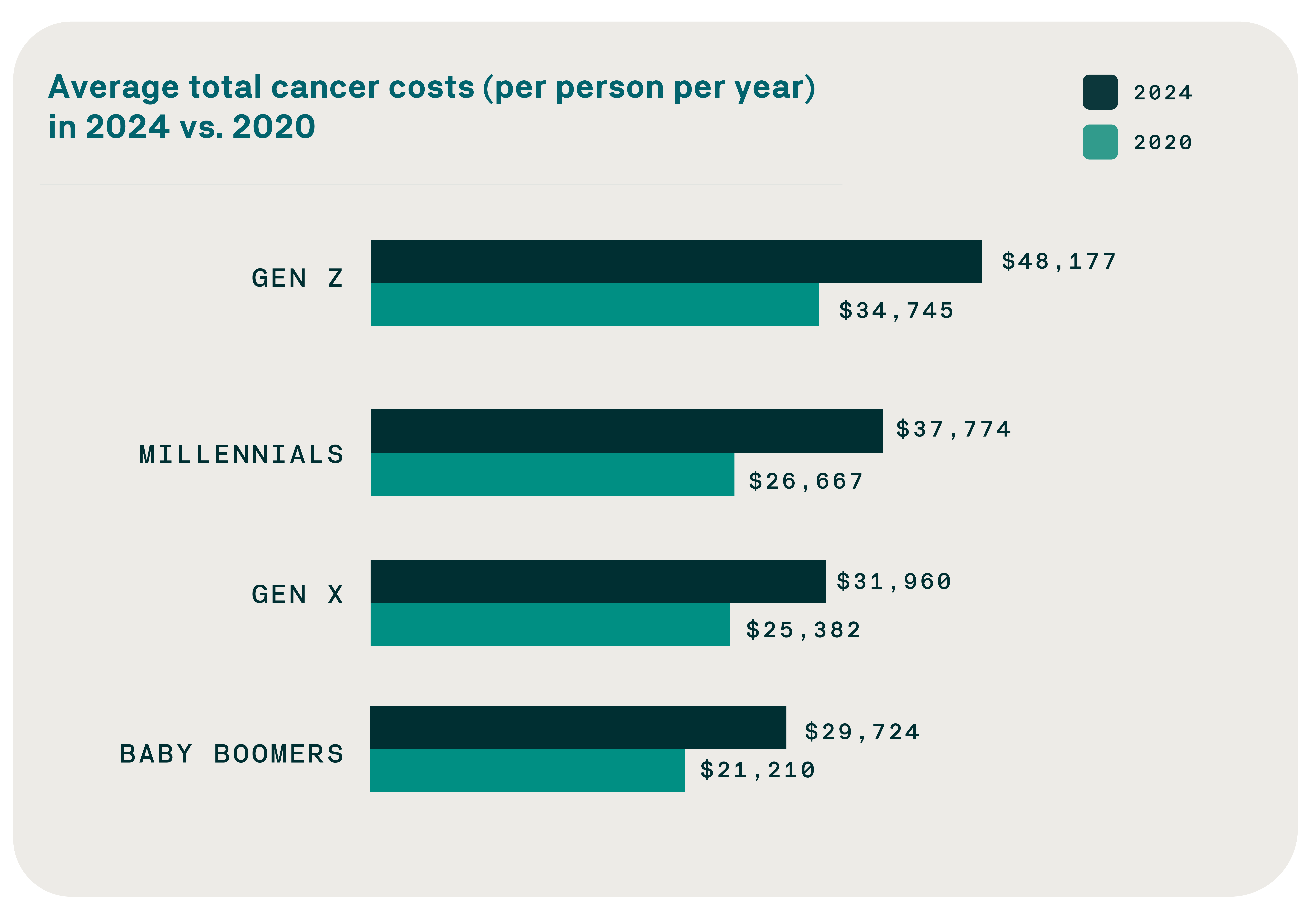
“For many younger patients, cancer treatment now includes long‑term use of specialty medications,” Raetz said. “Ensuring access to specialty pharmacy coverage alongside medical care is increasingly central to treatment continuity and affordability over time.”
Earlier diagnosis also changes the overall cost trajectory of cancer care. “It raises the stakes for early detection, appropriate site of care, and coordinated, value‑based treatment – not just for patients, but for employers and health plans,” Charania said.
The report also highlights a continued shift toward outpatient, drug‑driven cancer care, with specialty injectable therapies accounting for a growing share of health care spending. Where care is delivered – and how it is managed – has become a key lever for both quality and affordability.
Rethinking cancer care around today’s workforce
Taken together, the findings point to a need for modernization across the cancer continuum – from prevention and screening to benefit design and workplace support.
“Earlier diagnosis extends the cancer experience across much longer working lives,” Raetz said. “This means health systems and employers need strategies that account for years, not just months, of care, recovery, and support.”
Traditional age‑based screening models may not fully reflect emerging generational risk patterns. Likewise, fragmented health care models can leave younger patients navigating clinical, emotional, and financial challenges on their own.
“We need risk‑based screening, better navigation, and integrated support that reflects how people actually live and work today,” Charania said. “That means proactively bringing mental health, financial counseling, and caregiver support into the cancer journey, rather than treating them as secondary concerns.”
For employers, the report underscores the value of early detection, flexible workplace policies, and benefits that support employees over long care journeys. For the health care system, it highlights an opportunity to align innovation with access, affordability, and whole‑person care.
“Cancer among younger adults is no longer an anomaly, it is a growing reality, which calls for new ways of thinking about care, coverage, and compassion,” Charania said.
Evernorth Oncology Benefit ServicesSM simplifies and enhances the cancer care experience with an intelligent digital platform, a dedicated care team and access to a high-quality care ecosystem – all with a simplified, one-time payment structure for the patient. This patient-centric support is supplemented with virtual care and deep clinical pharmacy expertise from oncology specialists.


