Member Experience Insights Newsletter
Our Member Experience Insights Newsletter features must-see updates on our pharmacy benefit member experience innovations. Published three times a year, this newsletter provides a consistent, streamlined space to highlight key updates, upcoming opportunities and tools that deliver exceptional value to members.

The future of the pharmacy benefit member experience
Last year we shared our commitments to transforming experiences for you and your members. See how we’re delivering with greater choice, transparency and access. Stay tuned for new enhancements and experiences throughout the year.
Insights on our experience
Enhanced digital experiences are now live for most members, creating a more seamless and personalized journey. Communications, including letters and emails like the Prior Authorization initiation email, for commercial and commercial health plans started going live at the start of the year, and communications for Medicare Part D plans went live starting April 1, 2026.
See the full scope and learn how these updates improve price transparency, simplify benefit education and provide personalized guidance—at no additional cost to you or your members.

Transforming the prior authorization journey
Reimagining the Prior Authorization (PA) experience to be simpler, more transparent and more supportive for members
New emails when a PA is initiated
Real-time online tracking for status updates and next steps
Advance expiration notices to avoid delays in care
A new educational video explaining the process

Innovation for prior authorizations
We’re building on the work we’ve done in the PA space to enhance and accelerate the process for patients, providers and clients.
Expanded third‑party integrations to improve connectivity and reduce friction
Smarter digital experiences with proactive guidance and personalized alerts
AI‑powered PA processing for faster decisions and fewer manual steps
Smarter rules to reduce unnecessary reauthorizations, especially for chronic conditions
Unlock the full power of our enhanced PA experience with OnePA
Plans managing their own PAs can now unlock OnePA to deliver a more seamless experience. For an additional fee, OnePA provides the same intuitive tools and member communications available to plans that use Express Scripts for PA management.
Contact your account representative to get started.
A simpler, more powerful Check Coverage experience
Effective Q2 2026, members will benefit from an enhanced and more streamlined pricing experience across express-scripts.com and our mobile app with the upgrade of our Check Coverage tool. With this upgrade, Check Coverage becomes the single, simplified interface for viewing medication pricing and coverage details.
Consistent experience
Check Coverage now incorporates all previously available capabilities—delivered through a more modern, intuitive and transparent experience that aligns with Medicare and federal transparency requirements, including Transparency in Coverage (TiC). These updates will also appear on the Open Enrollment site, for plans using this tool, ensuring a consistent experience across both platforms.
Seamless transition
No action is required from you or your members—this enhancement will be completely seamless and all existing access points to our historical pricing tool will automatically route users to Check Coverage.
Synced with single sign on (SSO)
For plans using SSO to access our pharmacy benefit experience, your existing sign-on paths will continue to work, and any deep links will automatically redirect to the enhanced tool.
Explore real examples of the experience and find more information about this new tool.
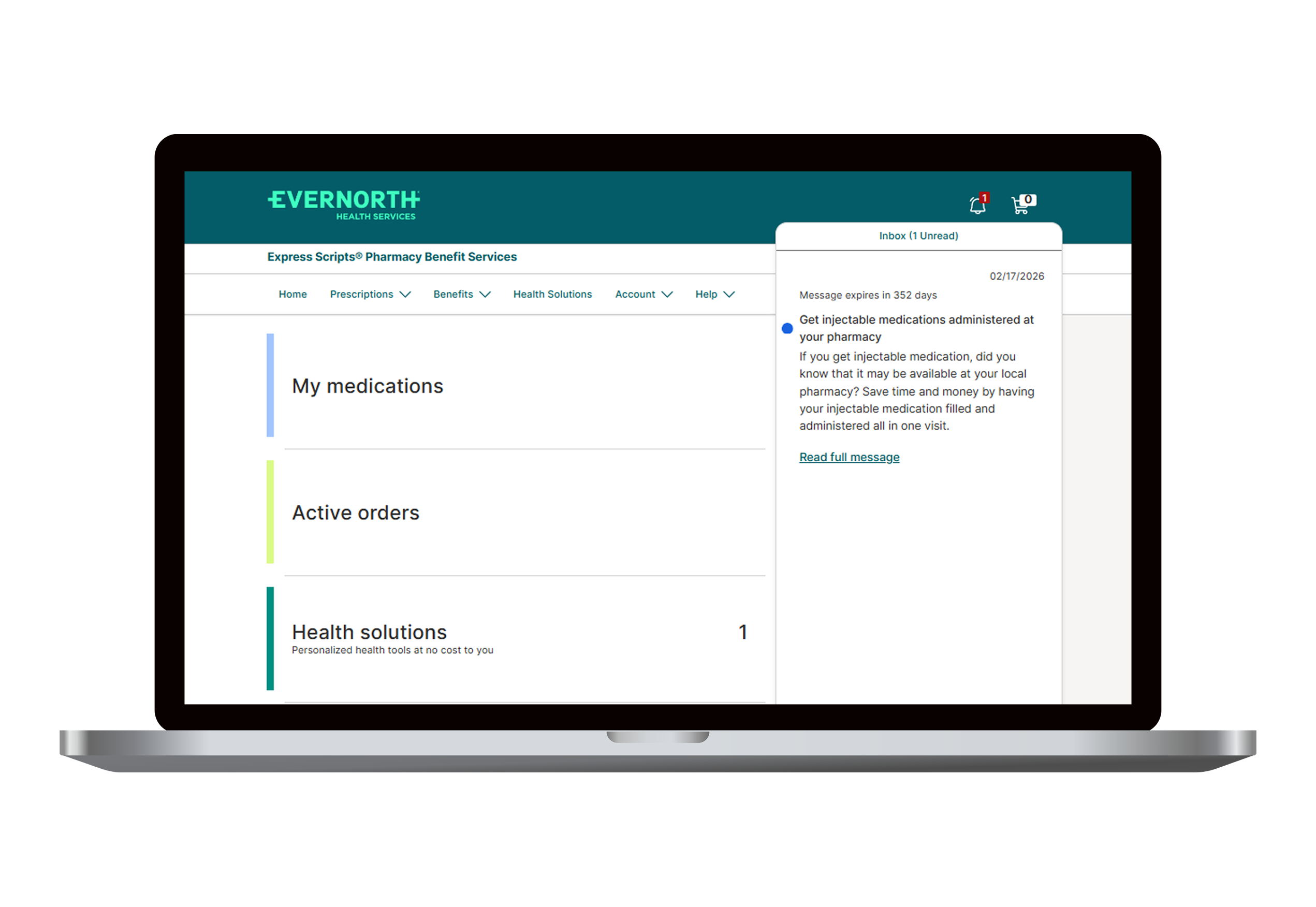
Instant, targeted messaging straight to members
Digital alerts give members the information they need, exactly when they need it. These quick, targeted messages can highlight pharmacy benefit details, seasonal opportunities like flu shot coverage, future plan changes, new plan year updates, benefit fairs and more.
Alerts are delivered directly to members’ inboxes and across key pages to ensure the right information arrives at the right time. Encourage your members to register on the member website to maximize the reach and impact of these digital alerts.
Delivering instant support with our AI-enhanced chat experience
After a successful pilot, our AI-powered chat* is ready to provide 24/7 access to quick answers for your members without ever picking up the phone.
Starting Q2 2026, we’ll begin introducing the experience, providing access to all members by January 1, 2027. This approach helps maintain quality, stability and a great member experience as access expands.

Enrollment details by line of business below. Please expand each section to review your enrollment options and opt-out details.
Help members get more from their benefits by powering up their digital experience
Drive stronger engagement and help members understand how they can get the most out of their pharmacy benefits with easy-to-use digital tools. When members sign up for an online account, they’ll be instantly connected to important information, smoother navigation and a more empowered experience.
Your new guide to understanding member experience
We support members with connected tools, communications and digital experiences. Our comprehensive journey guide shows you how we bring that support to life—from before their benefits begin through post-prescription support. Inside of this newly launched resource, you’ll find visuals of key experiences, sample communications, demos and more.
Contact your account representative for full access.

Building the future of pharmacy benefit experiences
The work doesn’t stop in 2026. See our plan for evolving the pharmacy benefit member experience through integrated experiences, personalized guidance, easier access to care and cost transparency. As we look ahead, we’ll continue introducing new enhancements and experiences—guided by member feedback, your input and proven practices from across different industries.

Footnotes
*Currently not available for Medicare Part D
**Details may vary by plan. While line of business differences are noted where applicable, some variations may not be reflected. All enhancements and visuals, which are representative of our strategic direction, are subject to change prior to launch. Digital experiences, functionality and timelines may change at any time.