Pharmacy innovation is at an all-time high. With countless clinical trials, improved diagnostic capabilities and groundbreaking therapies, people are living longer with fewer side effects. Despite the unprecedented upside, this evolution, or more accurately revolution, is adding complexity and cost to an already challenging landscape.
To help our partners better understand how to navigate these changes, Express Scripts® by Evernorth analyzed data and feedback from consumers, employers and health plan leaders nationwide. We compared the results from this survey to extensive research published by the Evernorth Research Institute, along with external trends from across the pharmaceutical industry. Our research uncovered three key areas at the forefront of pharmacy today. We developed our Pharmacy in Focus report to summarize these trends and help our partners develop strategies to address them in 2024 and beyond.
1. New innovations in therapy bring new challenges
Biosimilars, gene therapies and glucagon-like peptide 1 (GLP-1) agonists are just a few of the new therapies delivering never-before-seen health outcomes for members. But these innovations also bring additional cost, complexity and lack of predictability for plans and payers.
The rise of biosimilars
Biosimilars are powerful therapies derived from living organisms, such as blood, cells, tissues or proteins. These safe, clinically equivalent drugs are rapidly entering the market, offering a lower price themselves or forcing existing, name brand drugs to meet or even beat their price. This competition offers significant opportunity for the 52% of Americans with a chronic illness, because each biosimilar that enters the market promises better affordability for people paying for medication month after month. Pharmaceutical manufacturers are fiercely fighting to keep their formulas from being replicated by biosimilars. There are also legal and regulatory barriers that must be overcome before a biosimilar can be deemed as an interchangeable alternative. To take advantage of the savings biosimilars offer, payers must have a partner that can keep them informed of the clinical pipeline and regulatory updates.

Balancing budgets and access to gene therapies
Gene therapies carry million-dollar price tags that can bankrupt plans with a single claim. But for patients, a lack of coverage can put these life-changing therapies completely out of reach. While a claim hitting a plan may be uncommon today, there are more than 900 therapies in the pipeline for more common conditions. So now it becomes a question of when a claim will hit a plan, not if. Payers must be ready to offer these therapies for their population while protecting their budget.
Addressing cardiodiabesity with GLP-1 agonists
The soaring demand and subsequent shortage of GLP-1 drugs was driven by celebrity social media campaigns that touted their potential for weight-loss. That led to patients who needed these drugs due to a diabetes diagnosis struggling to access them. But should plans cover GLP-1s for weight loss alone? Despite their high price tags, GLP-1s could help curb the startling rise in obesity rates, leading to lower medical costs for people and plans down the road. With the number people living with a combination of obesity, diabetes and cardiovascular disease, otherwise known as "cardiodiabesity" climbing, investing in weight loss now could lead to lower costs in the future. A comprehensive strategy is needed for payers to protect their patients while controlling spend.
2. Health care affordability and accessibility are top of mind for consumers
Everyone is worried about the cost of medication. Even people with insurance are worried that their plan could decrease their coverage. That makes employers an important part of the strategy for keeping people safe. Because when members think they can’t afford their medication, they can go to dangerous lengths to save money. As challenging as the situation is for traditional patients, the obstacles and costs are even greater in the specialty space.
But it’s not just affordability that’s a challenge, it’s also access. Though people might live within just a few miles of a pharmacist, finding one that looks like them and understands their lifestyle is a consideration that’s moving to the forefront. We’re particularly seeing members of Gen Z voice this concern, which means this challenge could continue to grow in prominence for the future. Supporting small, local pharmacies, deploying copay support programs and connecting patients to pharmacists through technology will help bridge these gaps, but clients need the right pharmacy partner to make it happen.
Related: Social determinants of health play a bigger role than clinical care
3. Physician shortages call for the expanded role of pharmacists
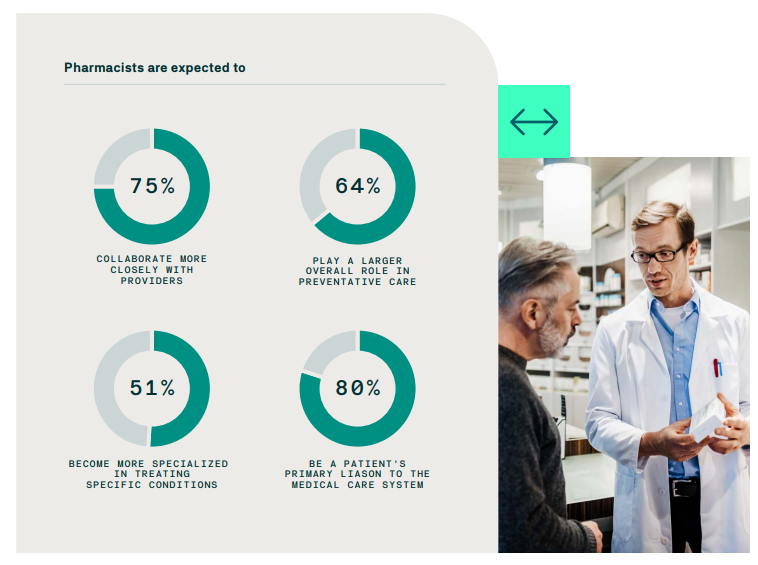
We could see the physician shortage reach 124,000+ in the next decade. And this lack of clinicians is coupled with a flood of new medical information. In fact, it’s estimated that it would take reading an impossible 29 hours per day to stay up to date on new medical research. To help supplement the shortage, providers see pharmacists stepping in to fill gaps in preventative care and become more specialized in treating specific conditions.
Related: The importance of expanding the pharmacist’s role in health care
But traditional pharmacists can’t be the only answer. According to the U.S. Bureau of Labor Statistics, there was a 6% decline in pharmacists working in pharmacies between 2019 and 2021. That’s why our Therapeutic Resource Center approach is becoming more valuable to clients, plans and patients. Our TRC pharmacists specialize in specific conditions and are able to stay up to date on the latest treatments and therapies entering the market.
As you work to address your biggest concerns, it's critical to have a partner that anticipates, understands and innovates around your efforts. Download the full Pharmacy in Focus report to see how Express Scripts by Evernorth is partnering, right by your side, to prepare you for the pharmacy trends we're experiencing today and developing strategies to keep you protected into the future.

